Patient is female diagnosed with Anaplastic Thyroid Cancer/ Metastatic differentiated carcinoma and in the past, Hx Lymphoma. Patient was very proactive in sourcing treatment and had just retired from work prior to her diagnosis and was enjoying retirement hobbies such as travel, gardening and home maintenance projects. In the beginning of the therapy she was diagnosed with Stage 1a LE – MDACC rating Scale (soft visible oedema, no pitting, and reversible)
Methods
Aim of the therapy was to reduce post-operative symptoms of swelling and post chemo/radiation effects of stiffness and fibrosis.
Therapy was started 7 weeks post radiation treatments. LymphaTouch treatment was conducted once per week in conjunction with regular lymphoedema therapy of MLD, Kinesio taping, compression therapy with foam inserts, SLD (self-lymphatic drainage). Patient reported good compliance with compression therapy but poor compliance with SLD. She was very compliant with attending clinic therapy sessions.
LymphaTouch® settings and techniques:
Pulse mode, default mode pulsation interval, 80mmHg – 120mmHg pressure range, 80mm, 50, 35mm Cups
Techniques included stationary and sliding with 80-60 mm cups for swelling, then 50 mm cup for lift and twist technique on fibrotic tissue
Results
At commencement of therapy we measured swelling with ALOHA circumference measures (Assessment of Lymphoedema of Head and Neck)
| Circumference (cm) Before Intervention June 12th 2020 | Circumference (cm) After intervention July 23rd 2020 | Circumference (cm) Follow up visit August 19th | |
| Lower neck | 41.5 | 36.7 | 37.6 |
| Upper neck | 44.4 | 40.8 | 39.0 |
| Ear to ear | 25.4 | 24.0 | 24.0 |
Swelling was also rated as MDACC rating scale for Lymphoedema (MD Anderson Cancer Centre). Patient rating remained at the same level as in the beginning, 1a – soft visible oedema, no pitting, reversible

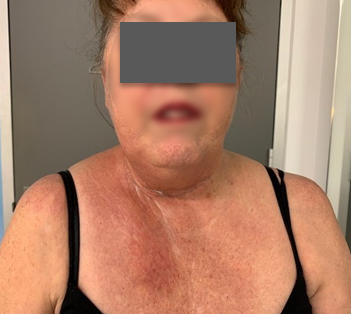
Before the intervention


After the intervention
Range of Movement of the neck was evaluated visually. Rotation improved by estimated 50 % compared to initial measure. Lateral flexion improved by estimated 20% compared to initial measure. In both direction, there was reduced movement towards left when compared to right side in the before the intervention.
Skin: Radiation induced telangiectasia was evident at supraclavicular and medial chest wall over sub pectoral nodal area (see photos). Colour and swelling appeared to have reduced over this area and contracted over the 6-week period.
Patient comment:
Patient commented that the therapeutic feel of the device was pleasant and acceptable. It afforded her improved range of motion after each session. She did comment that she particularly liked the LT therapy in conjunction with the other usual modalities of lymphoedmea therapy.
Case Report is from Chris O’Brien Lifehouse, Sydney, Australia
Sandra Templeton, Occupation therapist, Senior Lymphedema Specialist

